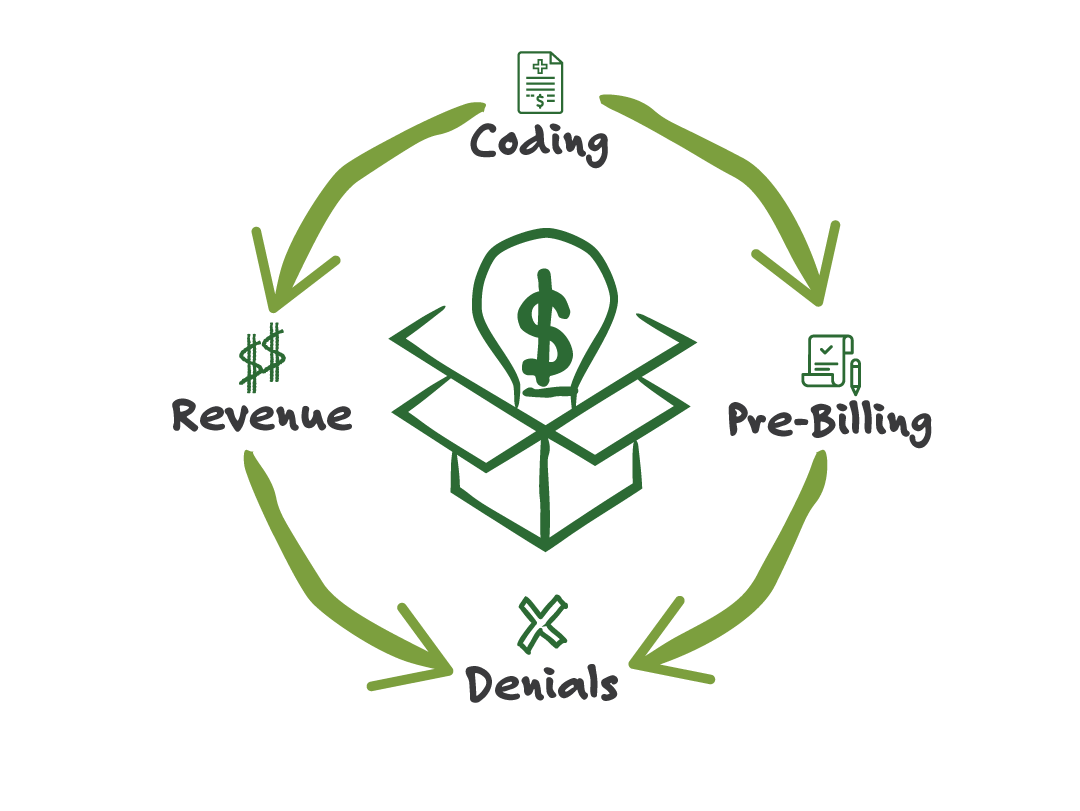
Solutions Spanning the Full Revenue Cycle
Coding & Claims Scrubbing
Our coding solutions guarantee accuracy and turnaround; is less costly and less hassle for hospitals, ASCs, and physicians. Use our long-term or temporary solution for eliminating backlogs, providing back-fill coding coverage. And our pre-billing solutions ensure that denials are minimized and revenue is optimized.
Denials Management
Lost Money from denied claims that have no resolution and never get re-billed creates a significant decrease in cash-flow. Unlike traditional coding companies, who just work the denials queue, we provide the expertise necessary to prevent denials from happening in the first place.

Revenue Capture
How do you know if you are capturing all your revenue? Our Revenue Capture services ensure your billing, coding, and reimbursement workflows & system configuration are optimized to maximize cash flow and minimize denials.
Contact Us & Learn How We Can Help
Coding Services & Claims Scrubbing Services
Our coding solutions guarantee accuracy and turnaround; is less costly and less hassle for hospitals, and physicians. Use our long-term or temporary solution for eliminating backlogs, providing back-fill coding coverage.
Our pre-billing solutions ensure that denials are minimized and revenue is optimized.

Coding Services
The cornerstone of our services are our coding services. Experience proves that an accurate coding process is the cornerstone to an optimized revenue cycle. Coding should be at the center of your RCM processes!

Charge Capture
We are able to conduct a comprehensive charge capture review in just a matter of hours, utilizing our proprietary toolset. We identify opportunities for improved charge capture, resulting in revenue capture findings for 100% of our clients.

Pre-Bill Scrubbing
We run six months of previously billed claims through our proprietary “e-scrubbing” system, which allows us to quickly identify the billing opportunities that have been missed which could result in increased revenue.

Claims Editing
Whether or not you utilize our claims scrubbing service, our team of experienced coders will perform & review claim edits in order to correct potential reasons for denials before the claim(s) are submitted, and implement revenue optimizations.
Denial Management Services
An all-to-common issue for provider organizations is the percentage of their claims which are partially or wholly denied by third party payers. Lost Money from denied claims that have no resolution and never get re-billed creates a significant decrease in cash-flow.
Unlike traditional coding companies, who just work the denials queue, we provide the expertise necessary to prevent denials from happening in the first place. We provide a “back-end” to “front-end” feed-back loop so that the front-end registration staff and the back-end billing and collections staff are communicating and tracking why these are denying. At the end of the day a “blue-print” or “road-map” is created that provides a solid solution to the decrease and the end of denied revenue.

Denials Improvement
We believe denials shouldn’t be an expected aspect of healthcare billing. Our services are focused on eliminating the reasons for whole or partial denials.

Claims Appeal Solutions
Many provider organizations lack the experience of how to effectively manage denied claims, which require navigating various 3rd party payer contracts. We bring the expertise necessary to optimize the claims appeal process.

Training & Education
It’s not reasonable to expect providers (and even billing staff) to know every aspect of the increasing complexities of coding. We provide education to providers as well as front & back-office staff.

Coding Compliance Audit
We provide a comprehensive (and time-efficient) review of coding related, billing and reimbursement practices aimed at identifying potential problems and stopping coding related denials.
Revenue Capture Services
How do you know if you are capturing all your revenue? Our Revenue Optimization services ensure your billing, coding, and reimbursement workflows & system configuration are optimized to maximize cash flow and minimize denials.

PPO Contract Review
We leverage our proprietary PPO Payment Audit/Assessment to identify and capture underpayments from payers and unauthorized Preferred Provider Organization (PPO) discounts.

Charge Master (CDM) & Fee Schedule Services
We conduct a comprehensive CDM or fee schedule review, developing a comprehensive picture of the current charging practices. From this, we implement improvements to eliminate inacurracies and maximize revenue.

Revenue Cycle Review & Practice Management
Our Practice Management Review/Assessment is the equivalent of performing a history and physical on your practice. Whether you think you are in wonderful shape, or are in significant financial or operational pain, we will take a look at your practice.

Third Party Payer Rules
ECS provides a review of all payer and medical policy rules on each patient’s claim before its filed. In order for a claim to be paid appropriately by the payer, each claim MUST be reviewed before its billed to determine if the claim meets medical necessity and other requirements. This also includes on how the claim should be billed to the payer according to their policy requirements.
ECS separates ourselves from other companies because of this process so that a claim(s) will not be denied. We perform this review on all audits that we perform, as well as, our revenue capture services. ECS calls this service “The Difference Maker”, the separation between us and our competitor(s).
E-Code Solutions
ECS delivers practical solutions and bottom line improvements to its customers, guaranteed.
© 2019 E-Code Solutions
MENU